ASSESSMENTS
Going Viral: The Geopolitics of the Flu
Jan 16, 2018 | 18:46 GMT
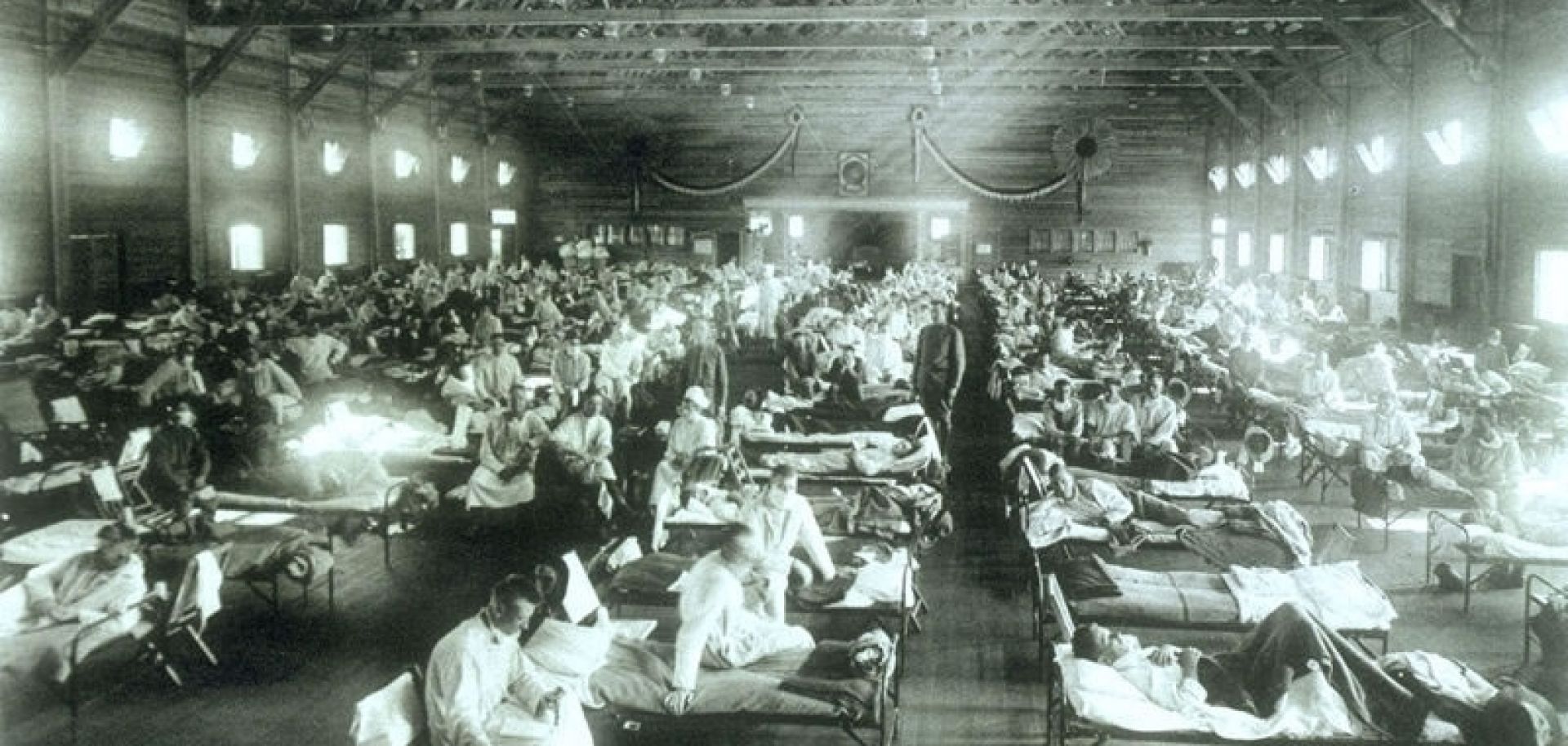
Sick patients fill the beds at an emergency hospital at Camp Funston, Kansas, during the 1918 flu pandemic. It is hypothesized that the flu began in southwestern Kansas and spread globally once it made its way to the nearby military training camp.
(NATIONAL MUSEUM OF HEALTH AND MEDICINE/AFIP)
Highlights
- On the 100-year anniversary of the 1918 flu pandemic, the Northern Hemisphere's flu season is poised to be a rough one.
- Medical advances and technology have helped people effectively combat a multitude of diseases, but the risk of a flu pandemic remains.
- Technological innovations in data analytics could help prevent the spread of disease, but they could face policy roadblocks.
Subscribe Now
SubscribeAlready have an account?
