GLOBAL PERSPECTIVES
What We Didn't Learn From the Ebola Outbreak

May 20, 2015 | 08:00 GMT
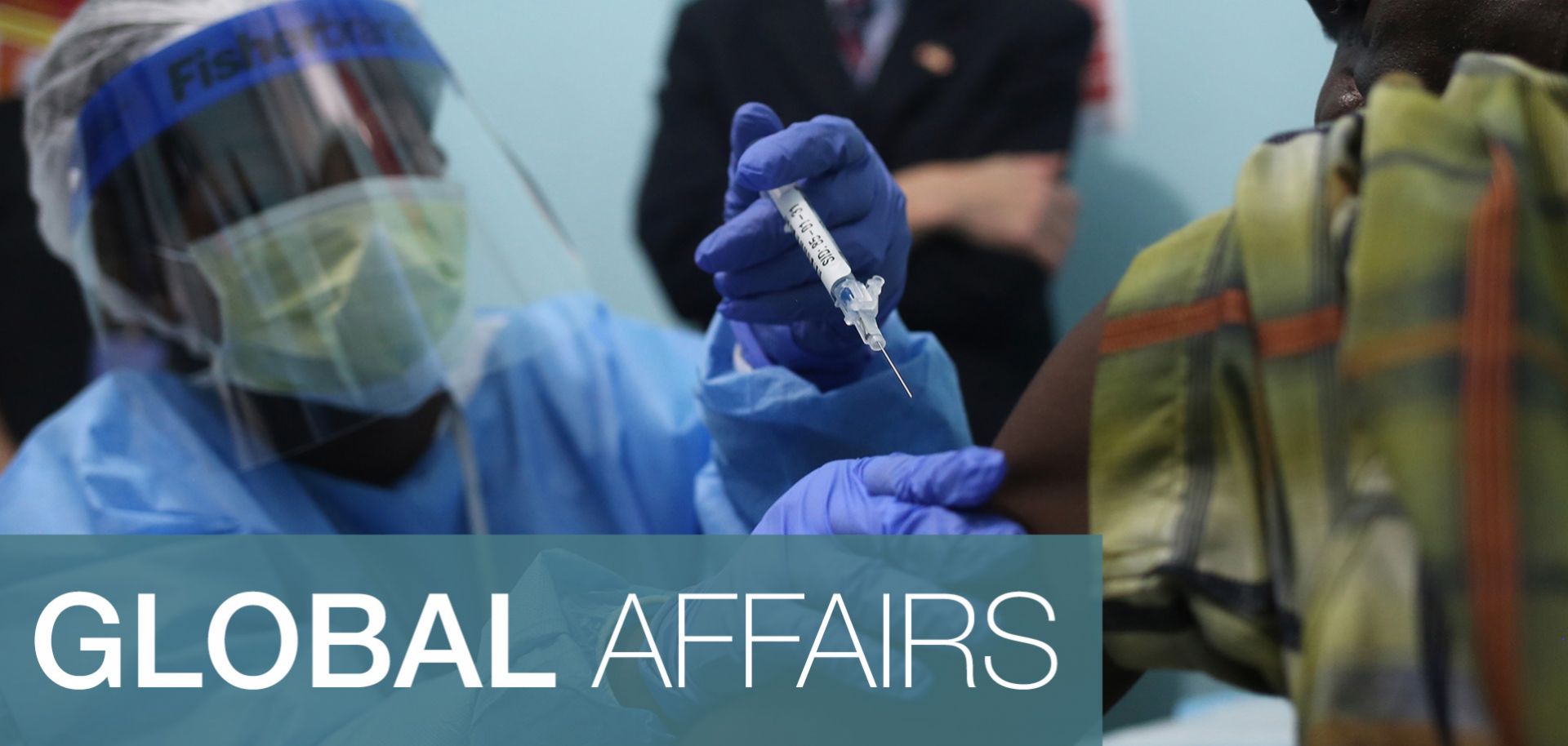
A nurse administers a trial vaccine during the first day of an Ebola vaccine study in Monrovia.
(John Moore/Getty Images)
Subscribe Now
SubscribeAlready have an account?
